In the fight against serious diseases and ailments, scientists often resort to the use of innovative technologies. As a result, hi-tech simulators have come to replace traditional therapy. If earlier many diseases and diagnoses sounded like a verdict, nowadays, the use of modern technologies gives patients hope for partial or even complete recovery.
Back in the early nineties, scientists began to master VR technology in medicine. Medical VR apps started to appear almost 20 years ago and included surgical simulators, rehabilitation applications, and telepresence surgery solutions in VR. One of the first VR simulators designed back in 1991 was The Green Telepresence Surgery System, which consisted of two units, the workstation for surgeons, and the remote worksite. Using such VR simulators, people could practice surgery with a scalpel and clamps, but on a virtual body. It was a huge step forward in medical education and capacity-building for surgeons.

Now, when virtual reality is rightly considered an integral part of many spheres of human life, medicine has not become an exception, and numerous studies in this direction are a confirmation to that. According to the research conducted by Research and Markets, the value of the virtual and augmented reality market in healthcare will reach $5 billion by 2023. Experts believe that virtual and augmented reality technologies will be widely used for treatment and rehabilitation purposes, diagnostics, and remote consultation of patients.
This research studies how virtual reality can be used in the rehabilitation of seriously ill patients. Besides, we’ll check some existing and potential applications for this technology in the field of disability and rehabilitation for the ease of reference.
Why to Use VR in Healthcare?
Today, Virtual Reality in medicine is nothing new, and there are more and more medical fields where the use of VR applications shows much better results compared with conventional therapy. The use of VR in rehabilitation has proved to be very effective, and for a good reason. Simulated virtual objects, environment, and events allow patients to plunge into an alternate reality, where they can interact with things and carry out actions not otherwise available to them in real life. This is one of the very few, if not the only, ways to let patients “escape” from the restrictive hospital environment.
Moreover, VR in rehabilitation:
- allows patients with different disorders to execute actions that they cannot perform in real life due to their disabilities;
- gives an opportunity to use more advanced digital rehabilitation methods as an alternative to traditional therapy, thus maximizing the effect of the rehabilitation measures;
- can be used in individualized treatment plans developed on the basis of careful assessment and following case-by-case treatment goals;
- helps analyze and better understand the needs of people with disabilities in public places and at home.

So, why is Virtual Reality ideal for rehabilitation?
In order to restore functions, the rehabilitation process should meet the following requirements:
- A patient should train in an environment that is as close as possible to the real world.
- A patient should be provided with timely feedback on the progress and quality of tasks he or she performs, so that he has the opportunity to understand and correct possible mistakes and redo the exercise as many times as possible until he succeeds.
- A patient should be engaged in the process and willing to be trained.
Using traditional methods, for example, therapeutic gymnastics, it is not always possible to follow all requirements, in contrast to VR. Virtual reality, with its capabilities to simulate practically any environment, the ability to provide fast and elaborate feedback along with highly motivational game-like tasks is able to fill the missing components of a successful rehabilitation program.
Virtual reality is a new way of rehabilitation through entertainment. It guarantees maximum involvement in the process promoting and encouraging patients to participate in treatment for maximum results.
Transform lives with our innovative VR therapy solutions. Start now!
Neurological Damages: VR Rehabilitation of Brain Injury and Stroke Survivors
Every year, more than 15 million people suffer a stroke and only a few of them manage to return to normal life afterward. The reason is obvious: stroke victims require a long and complex rehabilitation to be able to control their movements again and return to normal activity.
VR opens a wide field for the development of new rehabilitation methods for stroke and other brain injury survivors. VR affects involuntary movements produced automatically and on a subconscious level. Sensory stimuli of virtual reality cause muscle contractions and are effective in training balance, proprioception, and, especially, in restoring the paralyzed side of patients who have suffered a stroke.
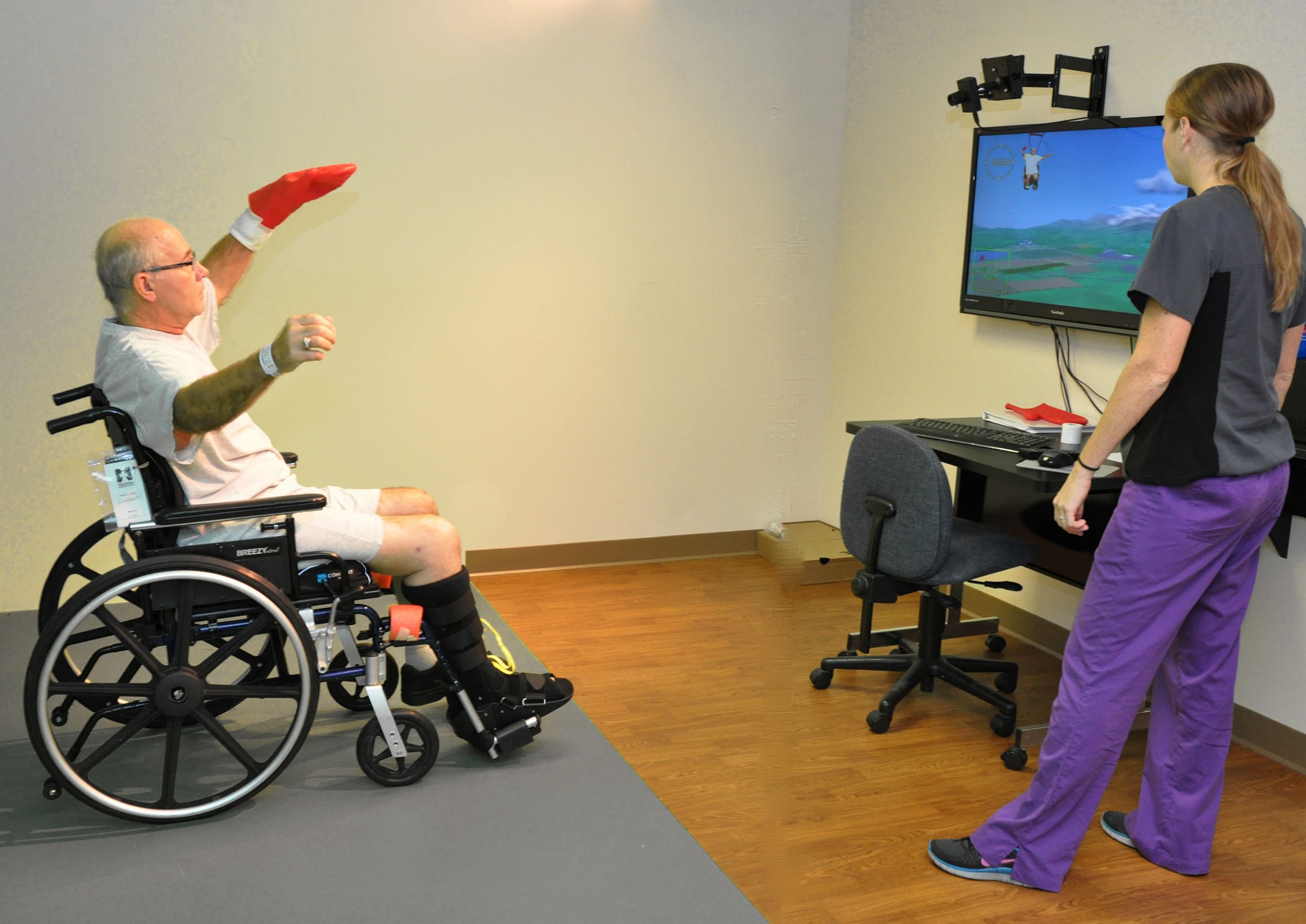
Rehabilitation programs that use virtual reality for recovery after a stroke demonstrate excellent results, improved psychological state, and increased motivation of patients. Here are some VR solutions that demonstrate an innovative and individual approach to the rehabilitation of brain injury and stroke victims.
IREX is an upper and lower-extremity exercise VR solution that uses video gesture control technology. The system helps patients restore multiple physical functions including balance, rotation, crouching, fine motor control, and others. The rehabilitation sessions are organized in form of a VR game resulting in a higher motivation of participants. Early studies of the IREX system showed that patients were up to three times more excited about rehabilitation with IREX compared to traditional rehabilitation procedures and were willing to repeat the sessions two or even three times in a row.
Restoration of Hand Motor Functions with VR
The consequences of circulatory diseases may seriously affect the quality of life of patients. The technology of virtual reality is also successfully used to restore the motor function of the upper limbs. One of the most important tasks in rehabilitation is to restore the basic motor skills of the hands, such as:
- ability to reach an object;
- manipulate it;
- coordinate the movements of both hands.
There are different causes of such disorders, but, primarily, they include muscle weakness and changes in the coordination of joint movements. Despite the fact that traditional physical rehabilitation of motor functions of hands can hardly be replaced by virtual therapy, some positive experiences of using the latter have already been accumulated. Though virtual reality has not found wide application in upper limb rehabilitation, multiple research in this domain indicate the greater efficiency of VR training compared with conventional rehabilitation, and some pioneering 3D solutions in this domain have been successfully adopted by US and European hospitals.
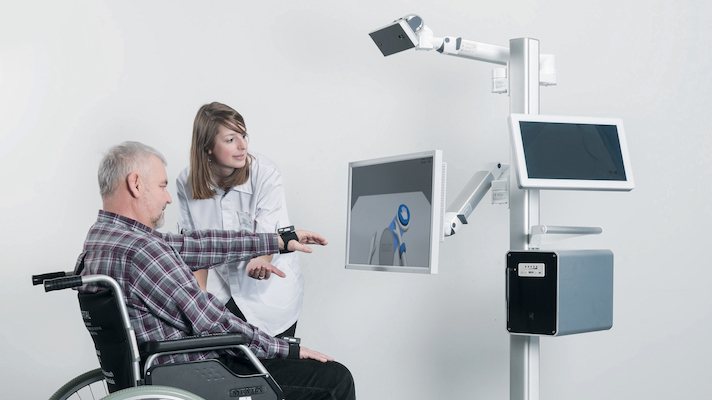
MindMotionPRO is a next-gen VR therapy system developed by a Swiss start-up MindMaze in close cooperation with neurorehabilitation experts. This system is used as an aid to restoring upper limb motor function as early as 1-6 weeks post stroke. The main benefits of this 3D solution include:
- enhancement of patient’s motivation with 3D virtual environments,
- immediate and illustrative feedback,
- improved outcomes through neurophysiological measurements & analysis.
MindMotion PRO has been developed over a decade by the neuroscientists and experts in VR and AR in Switzerland.
Restoring Posture and Balance with the Help of Virtual Reality
Virtual reality is widely used to rehabilitate patients with neurological disorders, especially to restore postural stability of patients with various forms of postural insufficiency .

Rehametrics is a VR system that uses the infrared camera of Microsoft Kinect for motion recognition. This platform can be used for clinical and at-home use to treat different physical and cognitive impairments.
Rehametrics allows to train in the form of a game or do functional exercises in a virtual gym. With Rehametrics, people can train static balance skills , endurance, unipodal balance, trunk control, and more. The uniqueness of this system is in its flexibility and possibility to adapt to individual treatment plans — an instructor or a doctor can adjust the range of available exercises individually for each patient.
VR in Post-Trauma Rehabilitation
People who suffer from pain and motion limitations after serious injuries now have a chance to rehabilitate with a next-gen 3D system CAREN .
This truly revolutionary, biomechanical VR system is designed for the rehabilitation of military personnel and athletes who have been seriously injured to help restore walking, posture and balance, and motor control, as well as recover from back pain caused by different injuries.


Both hardware and software components, including a motion base, motion capture, a projection screen, and the D-flow software are used by most advanced research centers and clinics to train and analyze different motor functions of patients. CAREN offers three default modes that can be modified further, depending on the specific needs and goals of patients in recovery.
VR in Rehabilitation of Patients with Post-Traumatic Stress Disorder
Immersion in virtual reality is one of the most effective ways to fight a post-traumatic syndrome disorder natural to militaries who experienced a traumatic shock during the hostilities. Some hospitals and military bases in the US use virtual reality programs, in which war veterans with similar psychosomatic disorders are plunged in simulated hot spots to go through emotional turmoil again, but in a safe virtual environment. This therapy allows releasing patients from bad experiences.

Bravemind is a virtual reality exposure therapy system used by hospitals and military bases to treat soldiers with post-traumatic stress. The BRAVEMIND VR Exposure Therapy software has significantly decreased combat-related PTSD symptoms. It allows soldiers to go back to hard memories, relive those moments again and again, but from a safe environment, and, finally, cope with their problems once and for all.
Virtual or Conventional Rehabilitation: What’s More Effective?
The possibility of virtual reality in medicine can be rightfully considered unlimited. The power of Virtual Reality is also used by architects to build hospitals of the future, where hospital wards and rooms, operating facilities and intensive care units, as well as comprehensive rehabilitation gyms and alternative therapies, are first tested in VR. As for the use of VR technology in rehabilitation, we would like to note that virtual reality, like any other high-tech method, has advantages and disadvantages in comparison to traditional methods of physical rehabilitation.

One of the obvious disadvantages of VR is the high cost of the equipment and software required to achieve the effect of a full immersion into a virtual space. But, despite some shortcomings, virtual reality has a number of undeniable advantages. The majority of patients involved in VR therapy were much more motivated compared to traditional physical rehabilitation. While going through rehabilitation sessions in VR, patients could try on different roles and perform actions hardly available to them in real life. Rehabilitation procedures with the use of Virtual Reality applications improve the emotional state of patients, which, in turn, serves as a further positive factor on the road to recovery.
It does not at all mean that virtual reality can replace traditional rehabilitation methods—of course not. However, we believe that virtual reality will soon take an important place in treatment and organically supplement conventional methods of rehabilitation.
























